Three weeks or so before I went into labor, I began having an odd feeling. It felt like the baby was sitting really low in my pelvis - I knew that I wasn't far enough along to be feeling that way so I called into the doctors office to explain. I spoke to a nurse and she felt like I was fine. I had just been in for an appointment a week or so before. I decided that it must be a normal sensation and chose to ignore it.
About a week before I delivered, I called into the Angel hotline (it was after five and the doctors office had already closed) to tell them that I felt like I needed to push. Again, they told me that it was probably fine.
.
.
3-15-10
I stayed at the school (I taught 1st grade at the time) until about 6:45pm working in my classroom. I felt unusually tired but it had been a long day. On the way to a school board meeting at 7pm, I met the school librarian, Faith Hendricks, outside of the administration building. She told me about a family member of hers who had gone into labor prematurely. This family member was already dilated to two centimeters. I asked her if the girl was scared and she said yes. I wish I had paid more attention to her story. That night I went home feeling bad, cramping a little but not enough to make me worried. I thought I was just tired from standing all day.
 I happened to get to work a little later than usual and I left a little earlier. During the day I was short of breath and had to sit down frequently. I had been cramping and mentioned it to the teachers at lunch. They asked if I had spoken with the doctor and I told them no. I was tired of bugging them about things that seemed to be normal pregnancy issues. I thought they were Braxton-Hicks contractions.
I happened to get to work a little later than usual and I left a little earlier. During the day I was short of breath and had to sit down frequently. I had been cramping and mentioned it to the teachers at lunch. They asked if I had spoken with the doctor and I told them no. I was tired of bugging them about things that seemed to be normal pregnancy issues. I thought they were Braxton-Hicks contractions.
That night I was really not feeling well. About 5:30pm I called the Angel hotline again and told them that I felt like I was cramping. The lady asked if I was having contractions and I said "I don't know, I've never had them before." To which she replied, "Oh, you would know if you were having them." She said I could go into into Labor and Delivery if I felt like I needed to or that I could wait until the morning to see my doctor. I called my mom and my brother (who is a doctor) and they both felt like I should probably go to the hospital. However, I hated to spend so much money for a false alarm. I wanted to wait to see if it would get better. I drank a few glasses of water, Michael made me a sandwich, and after determining that I felt a little better, we went to bed around ten.
3-17-10
Around 1:30 in the morning I moved to the couch - the cramps were getting worse. Moving didn't help. I decided to go back to bed. I woke up at 5am (my usual time) and went to the bathroom. My cramps were gone but I felt funny - I felt like I needed to push more than I ever had before. To my horror, I discovered blood while I was in the bathroom. I ran out of the room in a rush, told Michael that we needed to go to the ER, grabbed a few things off the floor to wear, and bolted out the door. Michael followed a few minutes behind me in his truck.
On my way, I prayed so hard. It was a twenty minute drive and each minute made me more hysterical...I began to cry and called my mom for consolation. We talked for a few minutes and she decided to come up to the hospital to be with me. I finally made it to the hospital and rushed through the doors. The receptionist pointed me in the right direction and I practically ran down the hallways. I came to an intersection where a group of nurses were having an animated conversation. Once they saw my face the conversation ended abruptly. One asked if I was ok...I nodded and continued down the hallway.
I walked in through the doors expecting to be forced onto a gurney and put on a monitor right away. A few nurses were sitting around talking again. I'm assuming that they were watching the monitors in front of them. They asked me to fill out a form while they looked up my information in the system. For some reason, they couldn't find my file so it took them a while to get to me. When I finally did lie down, we talked about my symptoms and then they hooked me up to a monitor and asked me to wait. My contractions had begun again on the way to the hospital. At first, they were light...but the longer I lay on my back the worse they became. As I was waiting I could hear the nurses talk amongst themselves about how many false-alarm preterm labor patients they had dealt with that night. They were deciding what to attribute it to....a full moon maybe? Suddenly I heard their voices drop to whispers. They were talking about me. I was scared and cold. I began to shake. A few minutes later one of the nurses came back to see me and told me that I was having contractions and that they were only two minutes apart. Michael came in around that time. The nurse called the doctor on duty and he told her to ask me a few more questions. Apparently he was going off duty and told her to wait for the next doctor to come on to examine me. In the meantime, I received a few shots to stop the contractions. After the third shot, it was obvious that they weren't helping. That's when they began trying for an IV. The nurse attempted to get a vein several times. She called in another nurse and she couldn't get one either. That nurse called in the anesthesiologist after a few attempts. Luckily he got a vein on his second try. By that point I was shaking even harder. They had tried about seven times to find a vein. My nurse came back around again and told us to expect to be there overnight at least.
A few minutes later, two techs came around to do an ultrasound. According to them, the baby weighed 1 pound 3 ounces. I asked them how dilated I was and they said that the ultrasound didn't show them. That was contradicted when, a few minutes later, the doctor finally made it in. She told me that the ultrasound showed that I was dilated to three centimeters and that my cervix was 100% effaced. She did a pelvic exam and told me that the amniotic sac was bulging out of the opening. She said that her goal would be to try to get my contractions to stop long enough to airlift me to Little Rock because they were not equipped to handle a 23 week baby (which was how far along I was at that point.) They put down the head of my bed to relieve the pressure in hopes that my water wouldn't break then began giving me magnesium sulfate through the IV (to stop the contractions.)
I was wheeled up to a room and given pain medication that I didn't ask for. I assume it was to help me relax and prevent more contractions. For a time, I lost track of things. My mom arrived sometime while I was sleeping. Michael and my mom tell me that a very arrogant neonatologist came by to tell us the statistics of mortality and morbidity for a 23/24 weeker. They were glad I missed out. Michael was so angry he nearly asked the guy to leave (which would be out of character for him.) Finally my contractions slowed enough for the doctor to consider airlifting. UAMS told my doctor that they would not take me if I was dilated more than 3 cm....so once again she did an exam. From what I understand of her remarks, I was closer to 4 cm by this point but she fudged it a little so that they would airlift me. We waited over an hour for the helicopter and the medics to come get me. They transferred me to a different bed and wheeled me out through the hospital. On a funny note, I think everyone in the waiting room downstairs got a good view of my backside as they wheeled me through....
I expected there to be more room in the helicopter once they put me in. There was just enough room for two medics, the pilot, and myself. They had to take off the fetal monitor. So instead, the woman medic listened for the baby's heartrate every 15 minutes or so until we landed. It was during the flight that my amniotic fluid began to leak. I thought for certain that my water was about to break in the helicopter. Thankfully, about 45 minutes later we landed and the medics wheeled me down to my labor and delivery room. During that transition, the male medic tried to sell me on naming the baby after him (they called him Buck but his real name was Phillip....no thanks.) When I made it into the room, things moved quickly. The nurses were assessing and asking questions. They also started another IV....which of course meant five more sticks and another anesthesiologist to get it done. The on-call neonatologist that night came to my bedside about the time that everyone was trying to find a vein. She came with an overly somber look on her face and watched for a moment while they dug around in my arm. She stood somewhere around my feet. She wanted to know if I knew the risk of having a baby at it's current gestation. I told her yes and she wanted me to tell her exactly what it meant. I told her that the baby could have serious complications and that it could die. She proceeded to give me the statistics, just like the doctor at the other hospital did to my mom and Michael. I stared at the ceiling trying to blink back the tears. About a fourth of the way through her speech I decided to focus my attention on the work being done on my arm. After all, what was I supposed to do about it? Keep the baby in? Well yeah, I was working on that. When she realized I wasn't listening to her, she paused., waiting for my attention - which I did not give. She stood around for a few minutes longer and attempted to continue a few times...hoping to get in a final word...then left.
Without my knowledge, I was given more medicine. I remember vaguely of a male doctor coming in and doing an exam. I don't know what he looked like or what else was going on in the room, but I do remember someone holding my hand very tightly. I asked the nurse later who was holding my hand and she said no one else was in the room. I asked Michael if he did it, but he hadn't made it to UAMS yet. I know for certain that someone was holding my hand. The doctor told the nurse that I was dilated to 5 cm and that my water was still intact. I don't remember much about the rest of the night. Michael and my mom got into Little Rock sometime around 8pm.
Without my knowledge, I was given more medicine. I remember vaguely of a male doctor coming in and doing an exam. I don't know what he looked like or what else was going on in the room, but I do remember someone holding my hand very tightly. I asked the nurse later who was holding my hand and she said no one else was in the room. I asked Michael if he did it, but he hadn't made it to UAMS yet. I know for certain that someone was holding my hand. The doctor told the nurse that I was dilated to 5 cm and that my water was still intact. I don't remember much about the rest of the night. Michael and my mom got into Little Rock sometime around 8pm.
3-18-10
By the afternoon, I still had not had contractions. They took me off the monitor. I was allowed to eat for the first time in two days. It was quite difficult having to eat upside down in my bed, but I managed.
After eating, I tried to sleep but I began having contractions again. The nurse came in and put me on the monitor for an hour or two. It wasn't showing much so they took me off. However, a few hours later I started to hurt and they put me back on AGAIN and found out that I was having about 4 contractions an hour. They weren't extremely painful but I felt terrified and discouraged every time I had one. I felt like I should be able to control my own body. I can't imagine how stressful it was for Michael to watch the contractions on the screen as I slept fitfully.
Sometime in the early morning I began to hear a sound....like someone drilling. My mom was already awake because of it and had called the nurse. The spotlight in the ceiling had begun to move around on it's own accord and it was making a ton of noise. Since I was awake, they decided to move me to a different room (which turned out to be right next to the resuscitation room where they put Samuel on the ventilator. I think it was a blessing that we were moved so close to that room...less time without air.)
3-19-10
In the morning I woke up feeling like I needed to use the bathroom. I was incredibly worried about having to go - I was feeling a lot of pressure and I didn't need my water to break. I laid there all morning thinking of any way I could avoid going. The previous few days I had the sweetest nurses. They were optimistic, full of encouragement, and listened to my concerns. The nurse I had that morning was the complete opposite. She was negative...gruff...and just generally rubbed me the wrong way. When I told her that I was feeling pressure she looked at me like "Ok....?"
The neonatologist on duty that morning was Dr. Ross (who would end up being Samuel's doctor.) He was the most positive person that we had spoken to about the situation. He asked me whether or not I would want to resuscitate the baby and I said "How could I not?" He told me that he felt the same way. It was a relief to talk to him and not Dr. Yap, who had spoken with me the day before.
An hour or so later, the two resident doctors on duty (a male and a female) came by to introduce themselves. The female doctor said her mom had told her about me - that there was a girl from Northwest Arkansas who was airlifted to UAMS. The doctor's mother had been praying for me. The guy doctor asked me how I had planned to deliver the baby. I hadn't realized that I had a choice. I had been told that a c-section would be better for the baby but because they would have to make a vertical incision, it would greatly diminish my chances of having children later. I told him that I would do what was best for the baby, but I would like to deliver vaginally if at all possible. The doctors left and my nurse came back in to let me know that I would have an ultrasound that morning to see if the baby had changed positions.
11:00am
The tech still hadn't arrived, so I ate lunch. I vividly remember the plate of fish they brought. It is an odd thing to remember. About an hour later, the tech came in and did the ultrasound. I had been lying on my side to relieve the pressure, but the tech wanted me to lie on my back. The ultrasound was very uncomfortable because of the pressure I was feeling. The baby was still breech. She told me that she could see the sack bulging and mentioned that it looked like the fluid was low. She also told me that according to her machine, the baby weighed more than it did a few days prior. She said he weighed 1 lb 9 oz. When she left, I felt even more uncomfortable. I tried my sides again but it didn't help.
1:00pm
I had been told that once my water broke, things would move quickly. I had no idea how quickly they meant. After the ultrasound, I decided that the best position for me lie in was my left side. My mom and Michael were talking in the corner and I was doing my best to try to forget how much pressure I was feeling.
I wiggled slightly in the bed and suddenly my water broke with an audible pop. It was the oddest feeling. I felt such a relief from the pressure that I was momentarily giddy. I told my mom and Michael what happened and it seemed like time froze. It was like all of us had to re-group for a second. My mom jumped up and hit the call button. A lazy voice came over the speaker asking what she could do. My mom told her what was happening and the nurse asked what room we were in. None of us had any idea and we looked at each other, wondering what to say. I think it finally clicked with the nurse what was going on. She said nevermind, the speaker went off, and suddenly the room was filled with at least fifteen people.
Michael and my mom came to stand somewhere around my head, and to my dismay, the male resident took the lead on the delivery. (I wasn't thrilled about having a male doctor...especially one that looked so close to my own age.) About half a minute later, he was telling me that the baby had already come down into the birth canal - still breech, booty first. He asked me what I would like to do. I remember saying "Just tell me what to do and I'll do it." I wanted what was best for the baby. I didn't feel scared...just tense and determined. I know that Michael felt the same way as he grabbed for my hand. My mom was holding on to Michael as she prayed aloud for me and the baby. The doctor told me that it would cause as much trauma to the baby to do a c-section now that he was already in the birth canal...so he opted for a regular delivery. A nurse I hadn't seen before asked the doctor if I needed a epidural or pain medicine. He said there wasn't time.
My nurse for the day (the bossy, negative one) took charge of the room at that point. They couldn't hear the heartbeat of the baby anymore and everyone was telling me that I had to get him out quickly. I remember thinking that I wish I had been able to take a few classes before delivering. I didn't even have time for a few practice pushes to figure it out. I still had ahold of Michael's hand at that point and I was told to begin pushing. The nurse yelled at me to let go of him, to curl up around the baby, and push. I finally figured out what I was doing and began making progress quickly. By this point the nurse was on top of me, pushing down on my stomach forcefully. I was worried that she was going to hurt the baby. Everyone in the room was yelling "Push, momma, push!" My nurse was practically in my face yelling it and I said, "I AM PUSHING!" She said something about how she knew and for me to keep pushing. If I had been in a better state of mind I might have backhanded her and told her that I was motivated enough without her help. I pushed for a grand total of ten minutes and the baby was out. The only thing I saw of him was his head full of hair as they ran with him out of the room.
While I finished in the room, my mom and Michael went to see the baby as they worked with him. They told me that they watched him shoot a stream of pee into one of the nurses pockets. Everyone was apparently thrilled that he had peed.
Michael and my mom came back after a few minutes, and not too much later, the staff wheeled the baby into the room. I was scared to see him. What would he look like? I had missed out on four months of bonding experience in the womb...would I love him? They wheeled to my bedside and I was surprised to see that his eyes were still fused shut. He didn't look as bad as I had imagined....but he certainly didn't look like a baby either. Dr. Ross, the neonatologist, told me that I could put my hand in the isolette to touch him. At that point I began to cry. I didn't know if I wanted to and at the same time I wanted to hold him so badly. This wasn't the way it was supposed to happen. You aren't supposed to see your baby, brought to you in a box...a machine breathing for it. Everything felt so surreal. I reached in and gingerly touched his hand. They wheeled him away from me and told me that I could visit him later. The crowd of people finally left my room.
5:00pm
The day of my delivery, I had several visitors come to give support - my roommate from college, my best friend from high school and her husband, my older brother and his family, my parents, and my younger brother. It was a relief to have them there. I spent the rest of the evening up and about.
When our visitors left, Michael and I went to see the baby before we went to bed. The hallway leading to the NICU had a "Wall of Hope" - consisting of pictures of normal, healthy children who were born exceptionally early. I couldn't look at the pictures. I wasn't ready.
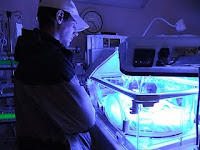
I was surprised to find that the baby had his own room. On the outside of the door, they had posted a sign that read 'BB Pope.' As we walked in, the nurse on duty followed us to the baby's isolette. I didn't expect to see the baby underneath a Bili light - I guess I assumed that they were only for full-term babies with jaundice. He was an odd red color due to the blood transfusion they were giving him. Beside his isolette there was a Christmas tree of medicine pumps. I remember that we were most concerned about his blood pressure and blood sugar those first few days. The nurse spoke to Michael only - as she had when I had visited the baby earlier in the day with my parents. I was becoming increasingly frustrated. Did they feel like I didn't need to know or couldn't handle what was going on with the baby? Finally Michael said something to the nurse about me being the baby's mother and she looked at me like she was seeing me for the first time. She said, "OH! I'm sorry. I didn't think you were the mother. Our moms usually arrive wearing pajamas and sitting in a wheelchair." I had changed into jeans and a maternity top that my mom had hurriedly packed me before coming down to Little Rock a few days prior. I felt relieved to know that I wasn't intentionally being ignored.
I was exhausted from walking around the hospital all afternoon so we didn't stay in the room with the baby very long. We went back to the recovery room and fell asleep quickly.
3-20-10
About four in the morning I woke up and couldn't go back to sleep. Michael was asleep in the uncomfortable hospital chair that was positioned close to the bed. I tried to get him to take my bed (I wasn't tired) so that he could get decent sleep for the first time in four days. He refused to take the 'patients' bed. I convinced him to share it with me. When he fell asleep I tip-toed out of the room and made my way to the NICU. The nurse on duty was an incredibly sweet lady who seemed to be in love with her job. As I walked in, she was busy doing a few things in the isolette. The baby wasn't moving and I learned that he was being given quite a lot of pain medication and sedation. I began to cry. The nurse pulled up a chair to the isolette, gave me a quick hug, and left me to be with the baby alone. I sat for an hour or so, just praying for him.
The first three or four days were a blur. We continued to get good reports from the doctors and nurses about how well the baby was doing - in fact, exceptionally well for his age. They even attempted to take him off the ventilator because he was breathing room air and trying to breathe over the vent. It didn't work, but they had plans to try again in a few days. I began to think that maybe I was further along in my pregnancy than I had originally thought. Everyone seemed surprised about how well he was doing. Of course, I did hear that notorious phrase "Never trust a preemie." - meaning that things can change at any time - but I tried to ignore it. During this time I never touched the baby. There was a "minimal stimulation" order put in - which meant that no one touched the baby unless they absolutely had to.
During the day, Michael and I stayed in the room with the baby. Most of the time we were researching baby names and talking through the past few days. We discussed several names. Samuel was never a name that we had considered before his birth but it seemed appropriate. It means, "one prayed or petitioned for." It was the only name that felt right to both of us. Michael was set on the baby's middle name being Charles - which is a family name. I was the hold up on naming the baby. I wanted to name him Samuel Caden - which means "little fighter."
Each night, Michael went to a sleep-room across the hall from the NICU, and I stayed in the baby's NICU room on the couch (only one of us was allowed.) The nurses came in every two to four hours to draw blood...I was too worried to be sleeping much anyway.
3-22-10
On the fourth day, Michael went back to work and I stayed with the baby. We knew we were going to be there for the long-haul. The doctor told us that we would be there until our due date (July 4th.) My mom stayed with me in Michael's place.
3-23-10
The fifth day was the turning point. After the doctor rounded, he called me over to his computer to point out the lung condition that was beginning to show itself on the baby's lung x-ray. He called it PIE (pulmonary interstitial emphysema.) He told me that the plan was to take the baby off minimal stimulation and begin to roll him on his sides - hoping that it would help open his lungs.
3-24-10
Day number six was probably the worst day of my life. The PIE was getting worse but otherwise Dr. Ross felt like the baby had been doing so well that it was time to begin feeding him my milk through a feeding tube. They began feeds in the early afternoon. The baby's vitals began crashing around 5. No one knew what was wrong. His blood pressure was lower than it had ever been. His heartrate and oxygen level were dropping...the alarms were blaring. Each time the alarm went off I felt sick. Things kept getting worse. Around 9 o' clock the nurse called in the on-call neonatalogist....who unfortunately turned out to be Dr. Yap (the neonatalogist on duty who spoke with me on my first day at UAMS.) The doctor ordered an x-ray. She told me that they were looking for 'free-air' (air in the abdominal cavity.) The first x-ray didn't show anything but it was obvious that something was causing the baby to be very sick. He continued to get worse. Around midnight, I couldn't handle much more. I hadn't slept more than a few hours at a time since the baby had been born...and it was all I could do to keep it together. I told the nurse that I was going to go to my mom's sleep-room. She gave me a very stern look because people aren't supposed to share a room - she was adament that we not break the rule.
My mom and I went back in the room and I called Michael to tell him what was going on. For relief's sake, we discussed the baby's name again and once again we disagreed. Sometime after the phone call ended, my mom asked me, "Don't you think you need to name him?" She voiced what had been going on in my head since speaking with Michael. We needed to name him and I felt like time was running out. I called Michael back and told him.
The next half hour was long and and stressful. I felt sick. Whatever I was feeling, I know it was that much harder for my mom to watch me go through it. I was praying with every spare moment and thought. I felt like I couldn't say enough to adequately plead my case to God. My mom and I had the toughest conversation that I have ever had. I told her that I wondered if I needed to let the baby go...if God needed to take him, then let Him take him. After a bit of thoughtful silence, my mom suggested that we go back into the room, lay hands on the baby, and pray for him. We went back in, opened the isolette for the first time, and we both put our hands on him. I prayed that if it was God's will to take the baby, then He should take him, but that I wanted more than ANYTHING to keep him. I loved him already. My mom prayed and we both cried. The hospital had given me a snoodle (a doll-like thing that I was supposed to keep next to my skin...then give to the baby so that it could smell me while in the isolette) which I had worn, but had refused to put in the bed with the baby for fear of germs. I suddenly felt like it was important that he knew me and knew that I was there...so I placed the doll by his body, closed the isolette, and we left.
It was getting close to three a.m. by the time Dr. Yap knocked on my mom's door. They had discovered free air in the baby's belly on the most recent x-ray. He had a perforated bowel...which probably began when they started feeding him. She said that he would need to be transferred to Arkansas Children's Hospital and may need emergency surgery. Someone handed me paperwork to sign - permission to transfer by ambulance and release of medical records. I was told that EMS would be there in the next thirty minutes to get him. Michael and my dad were on their way.
EMT arrived, and began asking me all of the baby's background information. They asked for his name and just as the nurse was about say, "He doesn't have a name." I said "Samuel Charles Pope." I can't describe how amazing it was to say his name for the first time.
While I waited for them to wheel him out, I whispered my prayers for Samuel aloud. The EMT crew asked if I wanted to ride in the ambulance over to Children's. The nurse looked at him like, "You aren't supposed to do that!" but no one cared. It was raining outside and by the time I made it in the ambulance, I was soaked.
We arrived at Children's a few minutes later (luckily, the hospitals are only a few minutes apart.) My mom and I were led to a small waiting room to wait for the surgeon to come by with paperwork. I was informed that they would not need to do surgery at this point, but they would need to put in an abdominal drain. I signed, the surgeon left, and I laid down on the uncomfortable waiting room chairs.
About five a.m. I was led into the room to see Samuel. I met the two nurses who were taking care of him. One was a young brunette with kind eyes. The other was a woman my mother's age, with reddish brown hair and a southern drawl. After a bit, I briefly left the room to pump, and came back to discover that my dad and Michael were in with the baby. I hugged Michael and burst into tears...for what must have been the tenth time in two days. The young nurse handed me a tissue and the older nurse continued to explain something to my dad. That older nurse was Carolyn....who later became Samuel's primary nurse. I believe it was nothing short of a miracle that she was working that night (she usually only worked days) and that she felt the desire to request to become Samuel's nurse.
We also met Dr. Arrington that night (Samuel's neotatologist at ACH) who just happened to be on-call. He also isn't known for working many nights. He took Michael and I into a back room and showed us an x-ray. He wanted us to know that he would do everything he could to get Samuel on his team. His team, Team 3, is the only team in the NICU that has consistent doctors. I'm fairly certain I would have gone crazy those four months without the consistency that team provided.
I began the blog a few days later with a recap of everything that had happened since arriving at Children's. To read those first posts, go here.